A recent animal study in Frontiers in Immunology showed intriguing results that tie together the olfactory system, immune system, cognitive function, and Alzheimer’s disease.
First a little background…
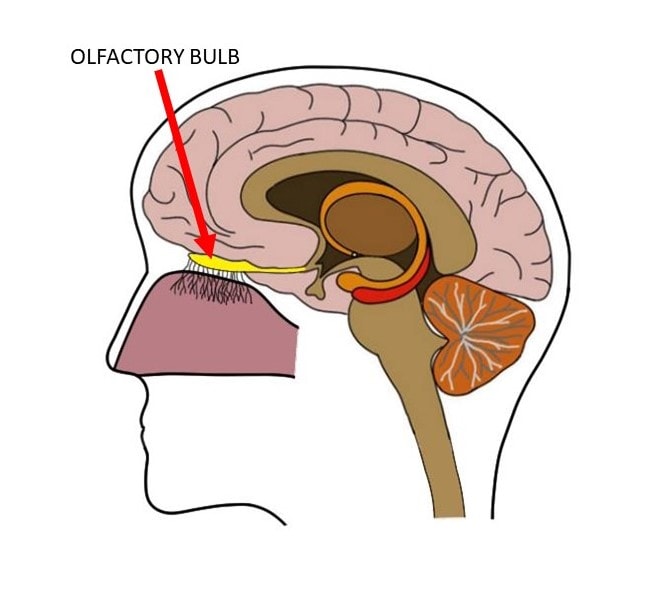
As odd as it may seem, both Alzheimer’s and Parkinson’s are related to olfactory dysfunction. For both diseases, a preclinical sign is hyposomnia, or decreased ability to smell odors.[ref] The epithelial cells lining the nose contain many different odor receptors. These receptors are connected via neurons to the olfactory bulb on the bottom of the brain.
Researchers have several theories about why hyposomnia is a precursor to Parkinson’s and Alzheimer’s, including neuronal damage by aggregated proteins in the olfactory system.[ref]
Back to this new study… [ref]
The researchers had previously found that certain odorants could either stimulate or suppress the immune system.
Exposing animals to menthol (such as in peppermint) drastically altered their immune response to vaccines. Plus, removing the olfactory bulb results in immune system changes as well as depression in animals.
Immune system activation in the brain seems to be an integral component to the pathology seen in Alzheimer’s and Parkinson’s.
The researchers used a mouse bred to have Alzheimer’s disease in the current study. They immunized the mice and then exposed the animals to menthol vapors for 15 minutes every 3 hours for 7 days. After the week, the mice were evaluated for cognitive changes and then sacrificed to check the immune response and mRNA changes in the brain.
The results were that the menthol odor exposure improved cognitive capacity compared to a control group. Additionally, there was a significant reduction in a couple of key inflammatory cytokines, IL-1B and IL-6, as well as CD3 in the prefrontal cortex. They also noted that the mice exposed to menthol had increased interferon-gamma production towards the immunization they had been given.
A pretty cool study. Let’s take a deeper look at other research tangentially related to it.
IL-1B is likely a key cytokine in the pathogenic processes of dementia. Genetic variants in IL1B are linked to an earlier age of onset of Alzheimer’s disease.[ref] In Alzheimer’s patients, IL-1B levels are elevated.[ref]
A link between periodontal disease and cognitive decline in aging exists. IL-1B is also elevated in patients “suffering from cognitive decline with pre-existing severe periodontitis.”[ref]
Inflammation in the brain is theorized to be at the heart of Alzheimer’s disease, with astrocyte activation playing a role.
TRPM8 is the receptor activated by menthol, and the TRPV1 receptor is blocked by menthol.[ref][ref]
Animal studies show that TRPM8 activation diminishes inflammation through decreased production of IL-1B, IL-6, and TNF-alpha. The mouse studies showed that genetically deleting TRPM8 abolished the anti-inflammatory effects of eucalyptus essential oil.[ref]
What to do with this information?
The obvious takeaway is that peppermint essential oil in an aromatherapy diffuser may give you more than just a pleasant smell. Peppermint essential oil contains about 40% menthol.[ref]
Is sniffing peppermint the cure-all for Alzheimer’s? I doubt it. But the immunomodulatory properties are definitely worth considering as part of an overall reduction strategy for neuroinflammation.
Considering the effects of the downregulation of IL-1B, alpha-lipoic acid may be a supplement to look into. Cell studies point to IL-1B and IL-6 being downregulated by alpha-lipoic acid.[ref]
